COVID-19 in Cardiovascular & AMI Care
A Time for Common Sense on How to Balance Evidence Based Medicine
and Processes with a
"Conscious COVID-19 Care"
-
COVID-19 Pandemic has significantly impacted the US healthcare systems and is a quickly evolving public health emergency.
-
In the last 3 decades we have significantly improved the management of acute myocardial infarction by the implementation of time efficient reperfusion strategies and systems of care for ST-segment elevation myocardial infarction (STEMI).
-
However, the last four months of COVID-19 pandemic has forced us to re-think and adapt to new process variables and how to balance the attention on treating Covid-19 patients, protecting others from the infection (including caregivers), while not losing perspective on serious non-COVID related diseases, such AMI.
-
This page provide multiple guidance documents and publications related to COVID-19 in cardiovascular and AMI care.
-
COVID-19 DASHBOARD LINKS (PR & GLOBAL) AT THE END OF THIS PAGE
American College of Cardiology Clinical Bulletin on COVID-19 Clinical Guidelines
-
ACC Clinical Bulletin COVID-19 Clinical Guidance For the CV Care Team.(Published: Feb, 2020)
-
This ACC clinical bulletin resource provides an overview of COVID-19, and outlines what is currently known from the published literature about the acute cardiac complication of COVID-19 and its implications for patients with underlying cardiovascular conditions. It also includes clinical guidance given current COVID-19 uncertainty, as well as recommendations for cardiac-specific preparedness.
-
To best serve your patients, protect yourself first! This is especially true for cardiovascular care team professionals that will be on the front line of the COVID-19 response. Use masks, gloves, and other personal protective equipment with discipline. Wash hands often. Decontaminate surfaces including stethoscope, cellular phones, computer peripherals, and other devices frequently.
American College of Cardiology & Other COVID-19 Related Guidelines & Publications
-
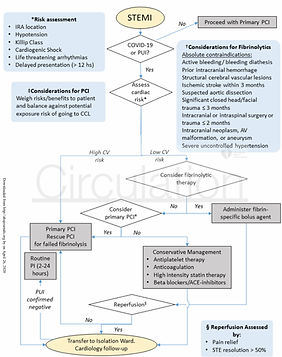
Reperfusion of STEMI in the COVID-19 Era- Business as Usual? (Published: JACC April 2020)
Proposed STEMI reperfussion algorithm for COVID-19 positive / or presumed positive (PUI).
Authors Conclusions: A blanket policy of PPCI for all STEMI patients may be hard to both justify and operationally deliver in the current environment when resources to protect the workforce are limiting, and systems delays may shift the balance in favor of fibrinolytic therapy (FT) strategies.
Candidates for FT? Should be considered for +COVID-19 or PUI, with a certain STEMI diagnosis, without extensive infarcts who present early (< 3 hours), without absolute FT contraindications.
FT may require a rescue PCI after 1- hour of clinical & ECG re-accessment. Exclusive COVID rapid testing may also be performed during the FT & reperfussion assessment to further determine the need for rescue PCI in a prepared Cath-Lab and team w full PPE.
-
Management of Acute Myocardial Infarction During the COVID-19 Pandemic (Published: JACC April 2020)
-
COVID-19 and Cardiovascular Disease (Published: Circulation Mar 21, 2020)
-
Cardiovascular Considerations for Patients, Health Care Workers, and Health Systems During the Coronavirus Disease 2019 (COVID-19) Pandemic (Published: JACC Mar 31, 2020)
-
Catheterization Laboratory Considerations During the Coronavirus (COVID-19) Pandemic: From ACC’s Interventional Council and SCAI (Published: JACC Mar 21, 2020)
Additional Interesting COVID-19 Publications
-
Reduction in ST-Segment Elevation Cardiac Catheterization Laboratory Activations in the United States during COVID-19 Pandemic.(Published: JACC April 2020)
-
Coronavirus Fulminant Myocarditis saved with glucocorticoid and human immunoglobulin (Published: Eur Heart J 2020, March 16)
-
The Untold Toll- The Pandemic’s Effects on Patients without COVID-19 (Published: NEJM April 17, 2020)
-
CPR in the Covid-19 Era--An Ethical Framework (Published: NEJM May 6, 2020)
-
Collateral damage: medical care avoidance behavior among patients with acute coronary syndrome during the COVID-19 pandemic. (Published: NEJM April- 2020)
-
STEMI care during COVID-19: losing sight of the forest for the trees (Published: NEJM April- 2020)
-
Pharmacologic Treatments for Coronavirus Disease 2019 (COVID-19) A Review. (Published: JAMA April 13/ 2020)
-
ESC Guidance for the Diagnosis and Management of CV Disease during the COVID-19 Pandemic (Published: ESC April 21, 2020)
Cardiovascular Involvement by COVID-19 (Published: ESC April 21, 2020)
Key points:
-
Severe COVID-19 infection is associated with myocardial damage and cardiac arrhythmia;
-
Monitoring of cardiac toxicity of antiviral drugs is recommended.
-
The pathobiology of coronavirus infection involves SARS-CoV‑2 binding to the host receptor angiotensin-converting enzyme 2 (ACE2) to mediate entry into cells;
-
ACE2, which is expressed in the lungs, heart and vessels, is a key member of the renin angiotensin system (RAS) important in the pathophysiology of CVD;
-
CVD associated with COVID-19, likely involves dysregulation of the RAS/ACE2 system due to SARS-CoV‑2 infection and due to comorbidities, such as hypertension;
-
CVD may be a primary phenomenon in COVID-19, but may be secondary to acute lung injury, which leads to increased cardiac workload, potentially problematic in patients with pre existing HF;
-
Cytokine release storm, originating from imbalance of T cell activation with dysregulated release of interleukin (IL)-6, IL-17 and other cytokines, may contribute to CVD in COVID-19. IL-6 targeting is being tested therapeutically;
-
Immune system activation along with immunometabolism alterations may result in plaque instability, contributing to development of acute coronary events.
-
ST-Elevation Myocardial Infarction in Patients with COVID-19: Clinical and Angiographic Outcomes (Published: Circ April 30, 2020; Stefanini G.)
Single-center retrospective analysis from Lombardy, Italy.
Objectives: Assess angiographic findings & pts. outcome
Data from all confirmed COVID-19 patients who underwent coronary angiography due to STEMI from February to March 2020 were analyzed.
24 STEMIs represented the first clinical manifestation of COVID-19
4 STEMIs during hospitalization for confirmed COVID-19
Key Findings:
-
The majority had localized wall motion on echocardiography (82.1%)
-
Culprit lesion was identified in 60% of the STEMI patients, while the rest had type 2 acute MI.
COVID-19 DASHBOARDS & CDC Website
COVID-19 Global Dashboard by the Johns Hopkins University
COVID-19 Puerto Rico Dashboard (Departamento de Salud, Gobierno de PR)
Centers of Disease Control and Prevention; COVID-19 Guidance Documents